September 23rd, 2015 •
1 comment

There seems to be a lot of confusion as to whether Adrenal Fatigue is actually the General Adaptation Syndrome (GAS) or not – or what the relationship is between the two of them. To make matters even more complicated some doctors and healthcare professionals refer to Adrenal Fatigue’s 3 Stages, 4 Stages, 5 Stages or even 7 Stages. So what is the relationship between Adrenal Fatigue and GAS and how many stages does Adrenal Fatigue have? In this first post I will give you my two cents on both matters and hope to clear things up for you. You will come to see that Adrenal Fatigue is actually a misnomer and a more accurate term would be HPA axis dysfunction.
Let’s start with a little history to provide some context
The definition of stress according to the dictionary:
Stress \stres\, noun;
1. Physical, mental, or emotional tension or strain
2. Importance or significance attached to a thing; emphasis
3. Physical pressure, pull, or other force exerted on one thing by another; strain
The term stress originates from Vulgar Latin “strictia”, from Latin “strictus” (tight, compressed, drawn together), passing through the Old French “destrece” , Middle French “destresse”, Middle English “distresses”, modern English “distress” and, by aphesis, became the modern word “stress”. The word was used in physics in the 15th century to mean applied pressure or physical strain and in the course of the 17th century the word stress began to be used to mean hardship or adversity. It would take until the early 20th century however, before stress took on its modern day meaning of psychological disturbance, ill health and mental disease.
In 1855 Thomas Addison discovered the adrenal glands and their importance in human health and disease. A little later George Beard (1839–1883), a noted American physician, posed that the newly imposed demands of the Industrial Revolution on 19th century life could cause an overload of the nervous system. In 1881 he coined this overload, neurasthenia, a weakness of the nervous system and nervous exhaustion.() Neurasthenia was characterized by symptoms of severe anxiety, unexplained fatigue and an inability of an individual’s nervous system to meet the demands of daily life. Sounds like Adrenal Fatigue, doesn’t it?
Dr. Henry R. Harrower, one of the early 20th century pioneering endocrinologists, surely seemed to think so and dedicated a section in his book to Neurasthenia, “Practical Organic Therapy, The Internal Secretions and the General Practice”.() This book was written shortly after World War 1, below is a copy of the entire chapter titled “Neurasthenia as an adrenal syndrome”:
“The minor form of functional hypoadrenia is more common than some have appreciated, and the fact that there is a psychic origin as well as the other physicologic causes already considered, allies it to the fashionable neurasthenia of today. In fact, some have stated that what is improperly called “neurasthenia” is not a disease per se, but really a symptom-complex of ductless glandular origin and that the adrenals are probably the most important factors in its causation. Campbell, Smith, Osborne, Williams, and others, including the writer, have directed attention to the importance of the adrenal origin of neurasthenia (though a pluriglandular dyscrasia is practically always discoverable), but so far this is not understood as well as its frequency and importance warrant”.
Besides the connection that Dr. Harrower made between Neurasthenia and Adrenal Fatigue, the 1915 quotation from the Journal of the American Medical Association also postulated a relationship between neurasthenia and low adrenal function. Quoting from the Journal of the A.M.A. ():
“The typical neurotic generally has, if not always, disturbance of the supradrenal glands on the side of insufficiency. The blood pressure in these neurasthenic patients is almost always low for the individuals and their circulation is poor. A vasomotor paralysis, often present, allows chillings, flushings, cold, or burning hands and feet, drowsiness when the patient is up, wakefulness on lying down and hence insomnia. There may be more or less tingling or numbness of the extremities”.
Remarkably, the ICD-10 system of the World Health Organization still includes neurasthenia under “F48 – Other neurotic disorders” (). Though it was omitted as a diagnosis in the American Psychiatric Association’s DSM in 1980 to be replaced by depressive and anxiety disorders and various psychophysiological and psychosomatic designations (one such condition that was added to the DSM in 1980 is the Post Traumatic Stress Disorder.) Neurasthenia to this day persists as an accepted diagnosis in Asia and is known in Japan as “shinkei-suijaku” (神経衰弱) and in China under the name of “shenjing shuairuo” (神经衰弱).
In the early 1900s, Dr. Charles Sajous, a medical doctor at Temple University, Jefferson Medical and the Medico-Chirurgical College in Philadelphia, continued the work of Dr. Addison by studying the glands. He was the first to use the term Hypoadrenia. He described Hypoadrenia as a state of adrenal gland “exhaustion” in which symptoms of fatigue and susceptibility to infection would arise as a consequence of prolonged strain or labor. He further distinguished 3 stages of Hypoadrenia dependent upon the degree of adrenal dysfunction.
- Functional hypoadrenia – adrenal glands unable to function properly
- Progressive hypoadrenia – internal assaults (like infections and cancer) progressively shut down adrenal gland function.
- Terminal hypoadrenia – “Exhaustion” of adrenal glands occuring as a result of the initial assaults.
When Walter B. Cannon (1871-1945), an american physiologist discovered the fight-or-flight stress reaction (1915) and the the process of homeostasis (1926), stress took on the modern day meaning of psychological disturbance, ill health and mental disease. The fight-or-flight stress response was later recognized as the first stage (acute stress response) of a general adaptation syndrome (GAS) postulated by the most prominent pioneer of stress research, Hans Selye, to be a universal stress response among animals.
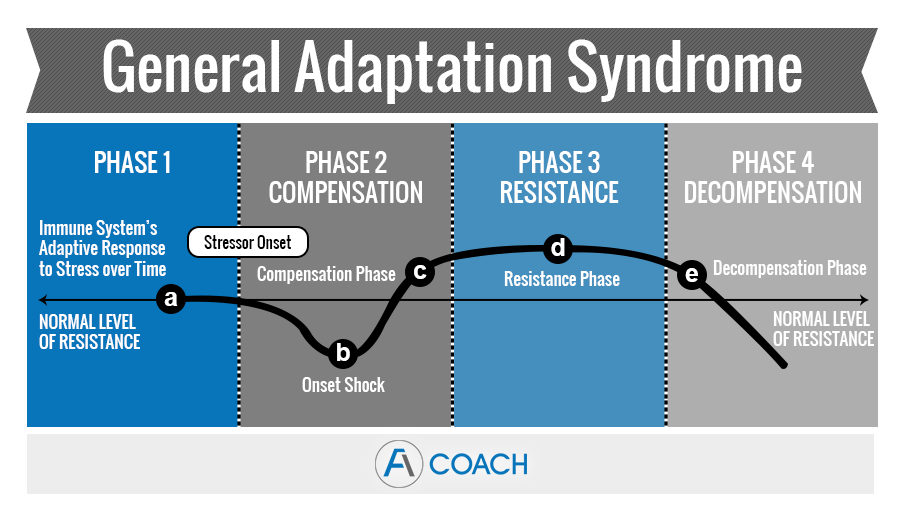
Hans Selye (1907–1982) described the General Adaptation Syndrome (GAS) in 1936, a biological explanation of how the body responds and adapts to stress. It involves three stages, the alarm stage, resistence stage and exhaustion stage. Transferring this to Adrenal Fatigue, there are many theories that explain how Adrenal Fatigue progresses through various stages of stress-related HPA axis dysfunction. These models are all loosely based on Hans Selye’s GAS theory of chronic stress in animal models and describe progressive stages based on adrenal hormone output measured in saliva (). The three-stage model is often cited, but there are also four-stage (see diagram below), five-stage and even seven-stage models to explain the progression of Adrenal Fatigue. Since Adrenal Fatigue is not a recognized medical condition there is no generally accepted model and doctors and healthcare professionals give their own twist to it acccording to their best understanding and clinical experience.
After World War II, several other physician-researchers continued the work of Dr. Sajous and Dr. Harrower, most notably Dr. John W. Tintera, Dr. Hans Selye, Dr. Gerald E. Poesnecker and Dr. James Wilson.
Dr. Tintera continued studying adrenal disease, in particular the relationship of adrenal malfunction to allergens and he advanced in 1966 the hypothesis that reactive hypoglycemia may result more from hypoadrenocorticism with deficient counterregulatory responses of the adrenal cortex than from insulin excess (, ).
Throughout the 1970s and 80s, Dr. Gerald Poesnecker, a chiropractor and naturopath synthesized all the late 19th and 20th century theories of adrenal deficiency, naming his disorder after Selye´s description and shortened it to Adrenal Syndrome. He referred in his books “It’s Only Natural” (1975), “Adrenal Syndrome” (1983) and “Chronic Fatigue Unmasked” (1993) to Chronic Fatigue Syndrome as “Adrenal Syndrome,” and utilize a saliva-based test that measures something they call the Adrenal Stress Index, or ASI. Dr. Poesnecker stated that CFS is truly a disorder resulting from inadequately functioning adrenal glands, while he stressed that it must be differentiated from organic adrenal insufficiency or Addison’s disease.
In 1995, Dr. Archibald Hart used the term “Adrenaline Fatigue” to refer to Hypoadrenia in his book, “Adrenaline and Stress”. He wrote: “…..when the adrenaline level remains high for an extended period of time, a state of “Hypoadrenia” – adrenaline fatigue – can set in”. Finally it was Dr. James Wilson, who in 1998 coined the term “adrenal fatigue” to identify below optimal adrenal function resulting from stress and distinguish it from Addison’s disease.
While, thanks to Dr. Wilson, the term Adrenal Fatigue has drawn much popular attention to stress-related diseases, critics argue that the simplistic nature of this term underestimates the complexity of the stress-response system by focusing solely on the adrenal glands and not accurately describing HPA axis dysfunction (Hypothalamus, Pituitary, Adrenal Glands). The HPA axis plays a pivotal role in triggering the stress response and not just the adrenal glands. In addition, because Adrenal Fatigue is referred to by many other names in medical literature (such as hypoadrenia, mild adrenal insuffiency, low cortisol state, neurasthenia) “Adrenal Fatigue” is mostly absent from peer-reviewed literature. This imperfect nomenclature would have also caused Endocrine Society to warn the general public against the “myth” of Adrenal Fatigue and to cast suspicion upon doctors and healthcare professionals using that term. ()
Granted, the term “Adrenal Fatigue” may not be accurately describing HPA axis dysfunction, but there is more than enough evidence that links failure of the HPA axis to habituate to chronic stress with adverse health outcomes (such as exhaustion, depression, anxiety and low self esteem , , ).
Although research over the past few decades has greatly increased our understanding of the role of the HPA axis and how acute and chronic stressors can create HPA axis dysfunction, most of that knowledge is either unknown or unleveraged within most healthcare settings today. Unfortunately there is no universal agreement on specific treatment and diagnostic measures to evaluate the wide range of HPA axis disorders.()
References & Further Reading














I really appreciate your article. The background and history of how we have presently arrived at the debate and conundrum of adrenal fatigue is so clear after reading. It looks like we need to capture a better “conversation” for discussing the physiological imbalances that occur from chronic stressors due to modern life.